 What is MERS?
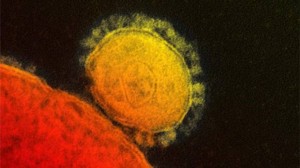
What is MERS?
MERS is in the family of coronaviruses.that includes the common cold.
The most severe coronavirus to date has been SARS (Severe Acute Respiratory Syndrome). SARS spread around the globe in 2003 and caused an epidemic that severely impacted economies as far apart as Hong Kong and Toronto.
As late as 2005, many hospitals around the world were still restricting visitors and checking all who entered through their doors.
MERS has not been seen in humans before. First detected two years ago, it was identified and named the Middle East Respiratory Syndrome last May. MERS, for which no known cure is available, destroys the lungs and kidneys. It is presumed that long-term physical contact can lead to infection.
MERS is not MRSA
Do not confuse MERS with MRSA (methicillin-resistant staphylococcus aureus) which is a strain of staph bacteria that is resistant to the antibiotics normally used to treat such infections.
MRSA is found in health care settings, affecting patients with weakened immune systems or those who had recently undergone surgery. Staph skin infections start off as a small, red bump that resembles a spider bite — these infections can progress quickly, turning into swollen, painful abscesses, which doctors need to surgically drain.
If the bacteria burrow deeper, they can cause infections throughout the body, including in the bloodstream, heart, bones, joints, lungs and surgical wounds, which can result in chest pain, fever and even death.
As a last resort, life-threatening MRSA infections can still be treated with the antibiotic vancomycin. However, new treatments may eventually be needed, as cases of vancomycin-resistant S. aureus are being reported.
FAQs from the World Health Organization
What are the symptoms of MERS-CoV?
Common symptoms are acute, serious respiratory illness with fever, cough, shortness of breath and breathing difficulties. Most patients have had pneumonia. Many have also had gastrointestinal symptoms, including diarrhoea. Some patients have had kidney failure.
About half of people infected with MERS-CoV have died. In people with immune deficiencies, the disease may have an atypical presentation. It is important to note that the current understanding of illness caused by this infection is based on a limited number of cases and may change as we learn more about the virus.
What is the significance of the recent finding of MERS-CoV in a camel?
On 11 November 2013, the Ministry of Health of Saudi Arabia announced that MERS-CoV had been detected in a camel linked to a human case in Saudi Arabia. This finding is consistent with previously published reports of MERS-CoV reactive antibodies in camels, and adds another important piece of information to our understanding of MERS-CoV ecology. However, this finding does not necessarily implicate camels directly in the chain of transmission to humans.
The critical question that remains about this virus is the route by which humans are infected, and the way in which they are exposed. Most patients who have tested positive for MERS-CoV had neither a human source of infection nor direct exposure to animals, including camels. It is still unclear whether camels, even if infected with MERS-CoV, play a role in transmission to humans. Further genetic sequencing and epidemiologic data are needed to understand the role, if any, of camels in the transmission of MERS CoV to humans.
See also
Glove Use Guidelines
MERS: Danger From The Invisible Medical Traveler
Links to track the progress of MERS
World Health Organization
Flutrackers
Twitter updates from
@MackayIM, @Crof, @Fla_Medic, @JATetro, @FluTrackers, @cmyeaton, @HelenBranswell, @MERS_inSAUDI, @Laurie_Garrett

 >
>